EHR System – Everything to know about
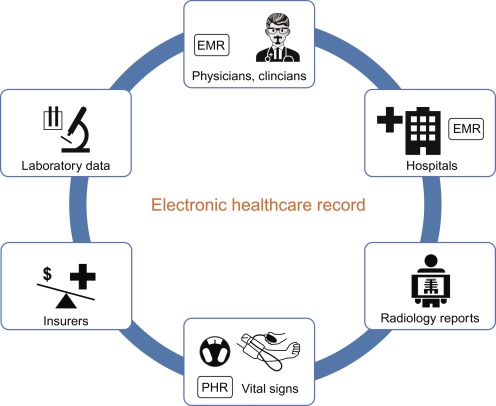
In the healthcare industry, adopting technology has transformed how healthcare is delivered. The electronic health record (EHR) system is one of the most significant technological advances in the healthcare industry.
Why do you need an HER System?
You must know how to build an EHR system. EHR is a digital version of a patient’s medical history that contains all the necessary information about a patient’s health, including demographics, medical history, medications, allergies, laboratory test results, and imaging reports. EHR systems are designed to improve the quality and efficiency of patient care. In this article, we will discuss the benefits of the EHR system.
Improved Regulatory Compliance
EHR systems can help healthcare organizations to comply with regulatory requirements. For example, EHR systems can help healthcare organizations to comply with HIPAA regulations by providing secure storage and transmission of patient information. EHR systems can also help healthcare organizations to comply with meaningful use requirements by providing the necessary data for quality reporting and performance improvement initiatives.
Improved Patient Care and Safety
tient care and safety in many ways. First, it helps to eliminate the risk of medical errors caused by illegible handwriting or incomplete medical records. The EHR system gives physicians real-time access to patient information, such as lab results and previous medical history, which helps make more informed patient care decisions.
Secondly, EHR systems can reduce the risk of medication errors by providing a comprehensive list of a patient’s current medications, dosages, and instructions. The system can also flag potential drug interactions, allergies, or contraindications, helping physicians prescribe medication more safely.
Improved Efficiency and Workflow
EHR systems can significantly improve the efficiency and workflow of healthcare providers. EHR systems can streamline patient registration and check-in, reduce the time required to retrieve patient information, and eliminate the need for paper-based record-keeping.
EHR systems can also help to reduce the time and effort required to document patient encounters, including progress notes, test results, and treatment plans. EHR systems can also help reduce the time spent on administrative tasks, such as billing and coding, thereby allowing healthcare providers to spend more time on patient care.
Improved Communication and Coordination of Care
EHR systems can help improve communication and care coordination among healthcare providers. The system provides a centralized location for all patient information authorized providers can access. This improves communication between primary care physicians, specialists, and other healthcare providers involved in a patient’s care.
The EHR system also allows for sharing of information between healthcare providers, including lab results, imaging reports, and other clinical information. This helps ensure that all providers are aware of the patient’s medical history, which can improve care coordination.
Data Analytics and Population Health Management
EHR systems can help healthcare organizations to analyze patient data and improve population health management. EHR systems can provide healthcare organizations with a wealth of data on patient health, including demographics, medical history, medications, and treatment outcomes.
This data can be used to identify trends in patient health and develop strategies to improve population health management. For example, EHR systems can identify patients with chronic conditions who are not receiving appropriate care and develop programs to improve their outcomes.
How to build an HER system?
Here, we will discuss the steps required to build an EHR system.
Step 1: Define the scope and requirements of the EHR system
The first step in building an EHR system is to define its scope and requirements. This involves identifying the system’s necessary features, functionalities, and workflows. The scope of the EHR system should align with the organization’s goals and objectives, taking into account the clinical specialties and workflows, patient populations, and regulatory requirements.
Step 2: Identify the stakeholders and secure buy-in
Identifying the stakeholders and securing their buy-in is crucial in building an EHR system. The stakeholders include clinical and non-clinical staff, patients, and external partners such as insurance providers and regulatory agencies. Engaging the stakeholders in the planning and design process ensures that the system meets their needs and expectations.
Step 3: Choose the appropriate EHR software
Selecting the appropriate EHR software is critical in building an EHR system. The software should be capable of handling the scope and requirements identified in step one and align with the organization’s goals and objectives. Other factors to consider when choosing EHR software include ease of use, scalability, interoperability, and security features.
Step 4: Develop a data migration plan
The EHR system should be designed to handle both historical and current patient data. The data migration plan should include steps for converting paper records and legacy electronic data into the new system. The data migration plan should also include a validation process to ensure that the data is accurately migrated to the new system.
Step 5: Configure the system
The EHR system must be configured to meet the organization’s needs and workflows. The configuration process includes defining templates, clinical decision support rules, and customizing workflows. The configuration should be done in a manner that enhances efficiency and does not compromise patient safety.
Step 6: Test the system
Testing the system is an essential step in building an EHR system. Testing should include a range of scenarios, from simple to complex, to ensure that the system can handle different types of patient data and workflows. User acceptance testing should also be conducted to ensure that the system meets the stakeholders’ expectations.
Step 7: Train the staff
The staff using the EHR system should be trained on how to use the system effectively. The training should cover basic and advanced features of the system, including data entry, navigation, and reporting. The training should also include policies and procedures for using the EHR system.
Step 8: Go live and monitor the system
Going live with the EHR system requires careful planning and execution. The process should include a phased approach to ensure the system is stable and meets the stakeholders’ needs. After going live, the system should be monitored continuously to promptly identify and address any issues.
Conclusion
Building an EHR system requires careful planning, execution, and maintenance. An effective EHR system can help healthcare organizations improve patient care, enhance communication and collaboration, and reduce costs.
Also read publicistpaper



